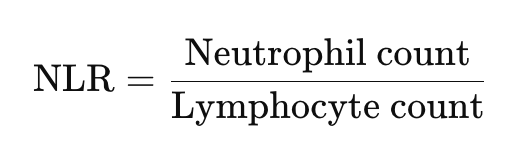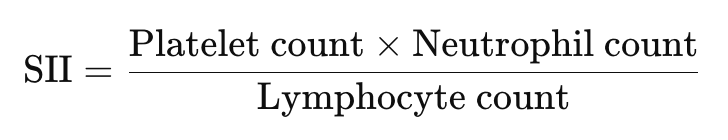Understanding Markers of Inflammation: hs-CRP, ESR, Ferritin, NLR, and SII
Chronic inflammation plays a central role in many health concerns — from cardiometabolic disease and autoimmune conditions to fatigue and hormonal imbalance. While inflammation is a normal part of healing, persistent low-grade inflammation can silently contribute to long-term tissue damage and increased disease risk.
Several blood markers can help us understand your body’s inflammatory state. Below are four key laboratory markers I often consider when assessing systemic inflammation: hs-CRP, Ferritin, Neutrophil-to-Lymphocyte Ratio (NLR), and the Systemic Inflammation Index (SII).
hs-CRP (High-Sensitivity C-Reactive Protein)
What it measures: hs-CRP is a protein produced by the liver in response to inflammation. It is one of the most sensitive markers of systemic and vascular inflammation.
Optimal range:
<1 mg/L: Low inflammation (optimal)
1–3 mg/L: Mild inflammation or early risk
>3 mg/L: Higher inflammation, often linked to metabolic, cardiovascular, or autoimmune processes
Clinical relevance: Elevated hs-CRP is associated with atherosclerosis, insulin resistance, metabolic syndrome, and chronic inflammatory conditions. It’s a helpful marker to track lifestyle and treatment progress over time.
Ferritin
What it measures: Ferritin is the body’s main iron storage protein, but it’s also an acute-phase reactant — meaning it rises during inflammation, even if iron levels are normal.
Optimal range:
50–150 µg/L: Generally healthy range for adults
Elevated ferritin (>150–200 µg/L) may indicate inflammatory or oxidative stress, liver dysfunction, or metabolic inflammation.
Clinical relevance: Chronically elevated ferritin can promote oxidative stress, damaging blood vessels and tissues. In metabolic and cardiovascular disease, elevated ferritin levels often reflect inflammation rather than iron overload, though both may coexist.
Neutrophil-to-Lymphocyte Ratio (NLR)
What it measures: NLR reflects the balance between the innate immune system (neutrophils) and the adaptive immune system (lymphocytes). It can be easily calculated from a standard CBC.
Interpretation:
1–2: Normal immune balance
2–3: Mild inflammation or physiologic stress
>3: Elevated systemic inflammation
>5: Significant inflammation (e.g., infection, cancer, or active autoimmune disease)
Clinical relevance: A higher NLR correlates with insulin resistance, endothelial dysfunction, and cardiovascular risk. It’s also being studied as a prognostic indicator in autoimmune and oncologic conditions.
Systemic Inflammation Index (SII)
What it measures: The Systemic Immune-Inflammation Index (SII) provides a more comprehensive picture of inflammation by incorporating platelets, neutrophils, and lymphocytes.
Interpretation:
<300: Normal
300–600: Mild inflammation
600–900: Moderate inflammation
>900: High systemic inflammation
Clinical relevance: SII reflects both platelet activation (a marker of vascular inflammation) and immune dysregulation. Higher values are associated with metabolic syndrome, atherosclerosis, autoimmune disease, and poorer outcomes in cancer.
ESR (Erythrocyte Sedimentation Rate)
What it measures: ESR reflects how quickly red blood cells settle in a test tube over one hour. When inflammation is present, proteins such as fibrinogen increase, causing red blood cells to clump together and settle faster. ESR is an indirect marker of inflammation and is particularly sensitive to chronic or autoimmune-driven processes.
Optimal range:
<20 mm/hr: low levels of inflammation
20–40 mm/hr: Mild to moderate inflammation
>40 mm/hr: Significant inflammation
>100 mm/hr: Suggests severe inflammatory or infectious pathology (e.g., autoimmune flare, temporal arteritis, malignancy, severe infection)
Clinical relevance: ESR is useful for identifying chronic inflammation, especially in conditions such as polymyalgia rheumatica, temporal arteritis, rheumatoid arthritis, and chronic infections. It rises more slowly than hs-CRP and is less sensitive to acute changes, but it can be invaluable for differentiating between acute and chronic inflammatory states or for detecting autoimmune disease.
Integrating These Markers Together
Each of these markers offers a unique lens into your inflammatory physiology:
hs-CRP shows general and vascular inflammation.
Ferritin reflects inflammatory or oxidative stress.
NLR captures immune system balance and stress response.
SII integrates multiple immune pathways for a broader view of chronic inflammation.
ESR highlights slower, chronic, or autoimmune-driven inflammatory activity.
When interpreted together, these values can provide valuable insight into cardiometabolic health, immune balance, and chronic disease risk — long before symptoms become severe.
Disclaimer: This information is for educational purposes only and is not intended to provide or replace medical advice, diagnosis, or treatment. Always consult your qualified healthcare provider for individualized recommendations.